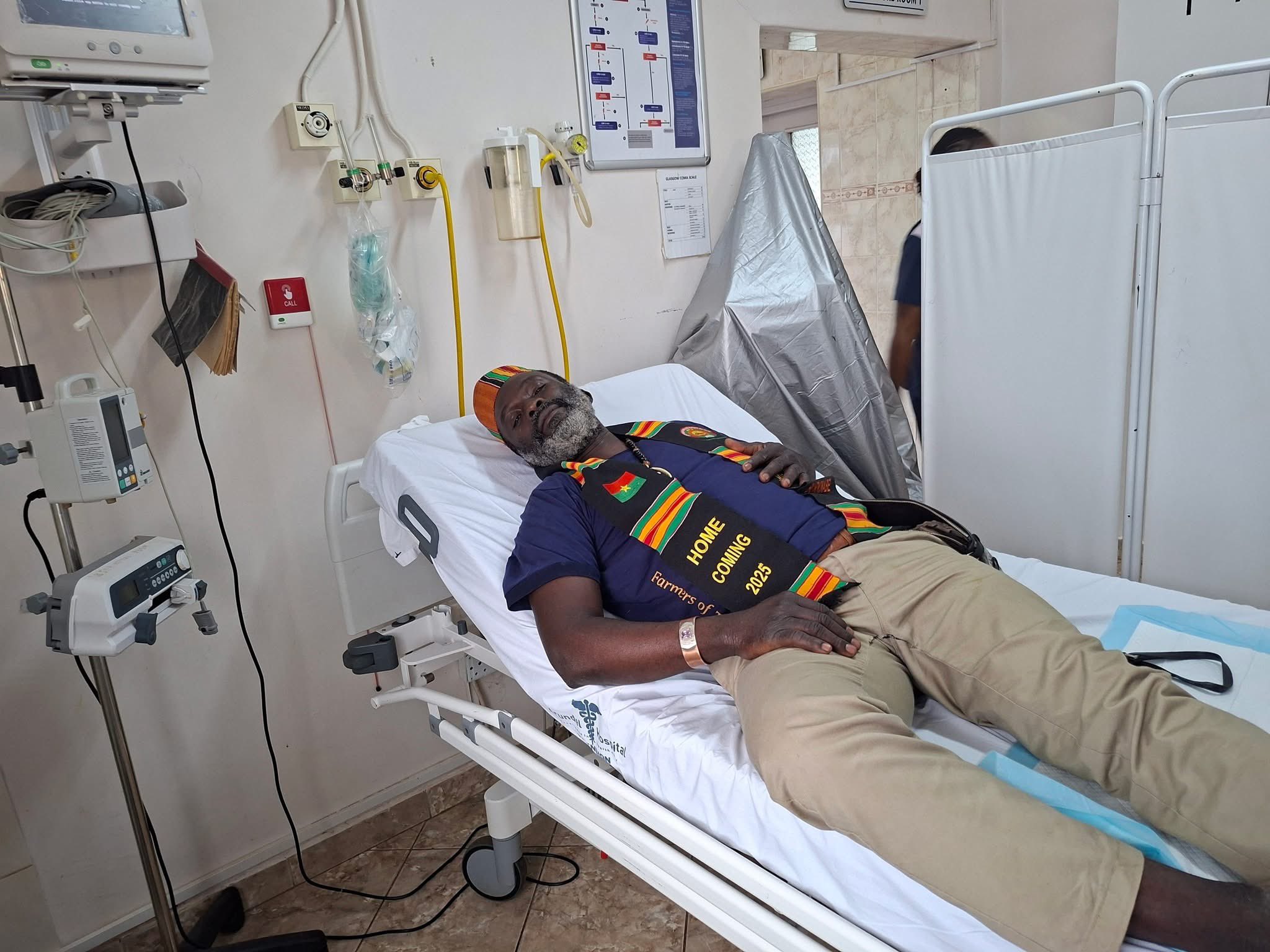
When public intellectual Joshua Maponga lay bleeding on the roadside near Kwekwe last week, he waited four hours for an ambulance that never arrived from the public sector. Instead, he was eventually transported to Arundel Hospital in Harare—a private facility owned by billionaire Kuda Tagwirei—bypassing multiple state-run institutions that lacked the basic equipment to save his life. This incident exposes a harrowing reality: despite the lifting of US sanctions on March 4, 2024, Zimbabwe’s public healthcare system remains a hollow shell, leaving citizens to rely on the benevolence of private oligarchs while the government prioritizes political longevity over life-saving infrastructure.
The Myth of Sanctions and the Reality of Neglect
For two decades, ZANU PF officials blamed Western sanctions for the systemic collapse of Zimbabwe’s hospitals. However, the removal of the Zimbabwe Sanctions Program by the US Treasury on March 4, 2024, has stripped away that shield. Historically, the health sector has suffered from chronic underfunding, with the 2023 budget allocation failing to meet the Abuja Declaration target of 15% of total government expenditure. Figures from the Zimbabwe Medical Association indicate that the country currently operates with less than 30% of the required ambulance fleet, a deficit that predates the 2023 elections but has worsened under the current administration’s fiscal priorities.
The Geopolitical Cost of Privatized Care
The reliance on private facilities like Arundel Hospital creates a dangerous precedent for Southern Africa. When the state abdicates its responsibility for emergency services, it shifts the burden onto a burgeoning private sector often controlled by politically connected elites. Dr. Tapiwa Muchena, a public health analyst, notes, 'The integration of political power and private medical ownership creates a conflict of interest where the state has no incentive to fix public hospitals because the ruling class is invested in the private alternatives.' This model threatens to destabilize the region, as Zimbabweans increasingly seek medical refuge in South Africa, further straining the already overburdened South African public health infrastructure.
The Human Toll of Policy Failure
The data is clear: emergency response times in Zimbabwe are among the highest in the SADC region. While the government now has the legal and economic freedom to lease modern ambulance fleets or import advanced medical technology, these resources have failed to materialize. The human cost is measured in preventable deaths. As Rutendo Matinyarare argues, the government possesses the liquidity to secure long-term lease agreements for ambulances and fire trucks, yet the political capital is being funneled into the '2030' campaign agenda. For the average Zimbabwean, the distance between a roadside accident and a functioning operating theater is not a matter of sanctions, but a matter of political will.
Voices of Dissent and Institutional Silence
Public frustration is reaching a boiling point. Social media discourse, led by figures like Matinyarare, has turned the spotlight on the administration’s post-sanctions performance. 'We fought for the removal of sanctions to empower our hospitals, not to enrich the political elite,' says one healthcare worker who requested anonymity for fear of reprisal. Conversely, government spokespeople maintain that the transition to a better health system is 'in progress,' though they offer no timeline for the procurement of essential emergency vehicles. The disconnect between government rhetoric and the reality on the ground has fueled a growing movement questioning the legitimacy of a term extension for the current leadership.
The Path Forward: Accountability or Stagnation
Looking ahead, the question remains: will the government pivot toward public health reform, or will it continue to prioritize political consolidation? Without a transparent, audited procurement process for medical infrastructure, the health sector will remain a symbol of systemic failure. The international community is watching, but the primary pressure must come from within. If the government fails to deliver basic emergency services, the legitimacy of its 2023 mandate will continue to erode, potentially leading to further civil unrest in Zimbabwe and increased migration pressures across the Southern African Development Community. The clock is ticking, not just for the patients on the roadside, but for the administration itself.